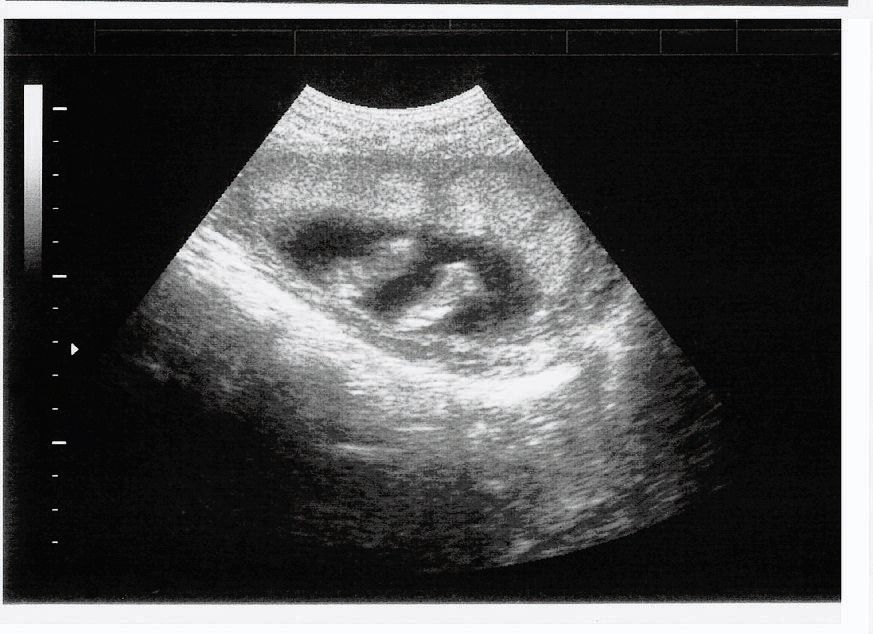
Three days of tallying
Why wasn’t I referred to a gynecologist when I mentioned I didn’t feel my son move as he did before? Exactly three months after Mikki was born we walked into the office of gynecologist Uittenbogaard once again for a second debriefing with our midwives. They repeat their conclusion: “We just overlooked a small baby.” But in the meanwhile, we’ve become familiar with the guideline ‘reduced fetal movements’ that states the subjective perception of the mother should be leading. The first time I mentioned I felt our baby move less there should have been excluded that there was something seriously wrong. The midwife should have referred to the gynecologist for an ultrasound. The instruction to tally for three days can’t be traced to any guidelines.
Why didn’t they tell us how important it is to take reduced fetal movement serious? After all a Norwegian study proved providing this kind of information leads to a decline in stillbirths, without an increase of unjust referrals. “When you provide this information, you get vastly differing reactions”, our midwife said. “You’re pregnant and vulnerable. Some women will leave with tears in their eyes saying ‘I won’t ever return to your practice’.” “That’s very patronizing, isn’t it?”, we say. Uittenbogaard: “Rather a tear than a dead child.” He makes the remark that we feel “unfairly reassured” and we affirm this. Midwife: “We are sorry you feel that way.” The midwives mention they will replace their reassuring folder. And that they will give referrals sooner next time when there are signs of decreased fetal movements.
“Would you do things the same way again?”, Uittenbogaard asks the most experienced midwife. “Well eh yeah, if I don’t have a clear picture I can’t establish if there really is reduced baby movement..” “Insane! That’s life threatening!”, we shout over each other.

Positive framing
Was this an incident, we finally ask ourselves. Did we by chance encounter a midwife that wasn’t knowledgeable enough about the guidelines, or is there more at play? In a 2012 analyses the Dutch Health care Inspectorate concluded that in 80 percent of deaths or severe complications occurring in ‘primary care’, “insufficient recognition of pathology” was the case. In 2015 systematic evaluations of infant mortality cases after 37 weeks of gestation between 2010 and 2012 revealed that in 20 percent of the cases obstetric care had failed, amongst other things because women weren’t being referred in time or at all, or because no ultrasound was conducted when suspicions of growth restriction arose. Gynecologists too, in 20 percent of the cases, fell short.
Midwives are trained to see a pregnancy as something normal. The KNOV encourages a ‘watchful waiting policy’. Midwives also have a financial interest in this. A midwife who assists a pregnant woman until the 29th week of gestation earns about 400 euros, if the assistance lasts until birth the midwife earns more than 1300 euros (even if there’s a referral during delivery). We requested the KNOV several times for an interview about infant mortality. To no avail; appointments are canceled and questions are routinely dealt with by mail due to “busy schedules”. Records of the General Members Assembly of June 12th 2015 shed a different light on this, we read: “The KNOV’s decision to not commit ourselves to media attention concerning infant mortality seems to be paying off”. “Instead the KNOV focuses on positive framing.”
In 2011 Minister Schippers instated the College of Perinatal Care to reform natal care in a manner that would decrease infant mortality. Together with representatives of all the professions chairman Chiel Bos (former chairman of the Dutch Health Insurance association) drew up a system in which midwives and gynecologists work together on risk selection in ‘birth centers’ which are closely aligned with hospitals. As to remove ‘perverse financial incentives’ from the system every health care provider receives a fixed amount per pregnancy. This system of ‘Integral Natal Care’ is to be introduced in 2017. The midwives professional association has also signed off on this.
But the midwives withdrew their support. The KNOV states in an email in an answer to our questions that the midwife should stay responsible when it comes to risk selection because “a lot of studies show” that it’s in the best interest of mother and child. Of course they discuss “high risk pregnancies” with other health care providers. “But if we have to discuss every woman that’s expecting in a maternity care team, unnecessary medicalization will increase and freedom of choice for the pregnant women will decrease. A GP doesn’t discuss all of his patients with specialists in the hospital now does he?” “When push comes to shove, the interests of the obstetric professionals aren’t that of the pregnant women but their own”, says Chiel Bos, “and of course they will go to great lengths to turn the tide.” Action group Geboortebeweging (Birth Movement), that highly values ‘natural’ birth, dismisses the attention for infant mortality as “pulling the dead baby card.” Last September, the KNOV hired an advisor for public affairs: Arjen van Berkel from lobbying firm EPPA, who, amongst other things is active in the tobacco lobby. Within four months after being appointed the Dutch Parliament (with 148 of the 175 votes) passed three motions to implement the integral maternal care “careful and in phases” and against medicalization.
At the General Meeting on the 31st of March, KNOV members voted against the new system in large numbers. Last week the KNOV withdrew confidence in the College of Perinatal Care and stepped out. Direct motivation was an interview where chairman Bos, as stated in a press release, “blames stillbirth on the midwives”. The professional association of midwives declares “to keep in dialogue with our partners in natal care.” The association of gynecologists NVOG called upon the midwives to reverse their decision: “We understand the emotions concerning the unfortunate statements of the CPZ chairman. Gynecologists have a shared responsibility when it comes to our relatively high rate of perinatal death. Walking away from the table doesn’t solve the problem, increases emotions and in the end will adversely affect pregnant women.”
In the consulting room
Since the end of March The United Kingdom, another country in which infant mortality is relatively high, has made stillbirth negotiable in the consulting room. The National Health Services published an action package called ‘Saving babies lives’ for professionals and pregnant women. The British flyer for women expecting clearly conveys the importance of feeling a baby move in the womb: “Around half of women who had a stillbirth noticed their baby’s movement had slowed down or stopped.” In Dutch flyers and consulting rooms the word ‘stillbirth’ is still carefully avoided. “Reduced baby movement could mean all sorts of things”, the KNOV spokesperson states. “You wouldn’t want to unnecessarily worry expecting mothers.”
Children like Mikki suffer the costs. Eight months old he would have been, instead we burn candles next to a tiny urn with his little mint green footprints on it, filled with three teaspoons of ash. Instead, we’re publishing this story. In the words of Paul de Reu: “Still too many babies die of the things-will-work-out syndrome.” In a response our midwives stated: “The stillbirth of your son impacted us greatly and has been on our minds a lot the last few months. We consider your decision to share your experience a positive one. We support it because, like you, we serve the interest of reducing infant mortality. […] Due to our professional confidentiality we cannot react substantively.”
HOW DO YOU DETECT IT?
The big challenge when detecting growth restriction is to distinguish between small fetuses who are healthy and those who are growth restricted. At the end of 2015 a British research group published (in The Lancet) a promising way to do this: by using ultrasounds to not only monitor the weight of the fetus but also the abdominal circumference of the unborn child – because a relative decrease of circumference indicates emaciation. Using this method they managed to cut the ‘false-positive’ diagnoses by half: for every correct diagnoses there’s only one incorrect one. This would greatly alleviate concerns pertaining to over-treatment and unnecessary premature births. The research group wants to make haste setting up a comparative study to confirm if their method actually does reduce infant mortality due to growth restriction.
BIRTHS ARE OFTEN PAID FOR TWICE IN THE NETHERLANDS
If a midwife refers a woman to a gynecologist during labor, both caregivers will be paid for the delivery. This measure was introduced in 1962 to prevent midwives postponing referrals. Downside to this is that midwives have a financial incentive to keep pregnant women under their care until these women go in to labor and only referring at that time. The referral rate during labor is around and about 39 percent these last few years (from 31 percent in 2000). Figures from the Dutch Health Authority (October 2015) show that midwives and gynecologists declare about 215.000 deliveries on a yearly basis when there are only 170.000 births. This means there are 45.000 deliveries being declared twice. Midwife Pien Offerhaus shows in her thesis from 2015 that the increase in referrals did not lead to a decrease in infant mortality or complication occurring with mother or child. Most significant reasons for referral are requests for anesthesia, meconium in the amniotic fluid and non-progressing dilation. Offerhaus names growing fear for complications as an explanation.
This article has been made possible by contributions from Boy Tripfonds voor Wetenschapsjournalistiek van het Fonds Bijzondere Journalistieke Projecten (the Boy Trip Foundation for Scientific Journalism of the Extraordinary Journalistic Projects Foundation). It was published in Dutch on April 22, 2016 in Dutch national newspaper NRC Handelsblad and NRC Next. On Wednesday November 16, 2016 the story was awarded the AAAS Kavli Science Journalism Gold Award, category large newspaper.
Appreciate this article and my work? You can now donate and keep me busy.
If you like this article and want to show it by giving a small (or big) donation, that’ possible. This way, you’re helping independent (science) journalism to maintain and flourish.
